Automate your healthcare phone calls
Automate phone call workflows across patient access, clinical operations, and revenue cycle management
Automate phone call workflows across patient access, clinical operations, and revenue cycle management
AI Agents can handle all major call center workflows without need for human involvement
Artificial voice and reasoning finally feel human-level, unlocking new levels of personalized patient engagement
Tensor automates workflows across patient access, clinical workflows, and revenue cycle management.

Save time taking patient's information and scheduling appointments over the phone.

Automate your prior authorizations -- for good. When all else fails, and you need to pick up the phone, now you can delegate those calls to Tensor.

Instead of reaching for the phone to verify elegibility and benefits, send it to our AI to handle.

Tensor automatically follows up – calling the payor to get updates on outstanding requests.

Free your nurses up from hours of tedioius calls to patients. Let Tensor handle them.
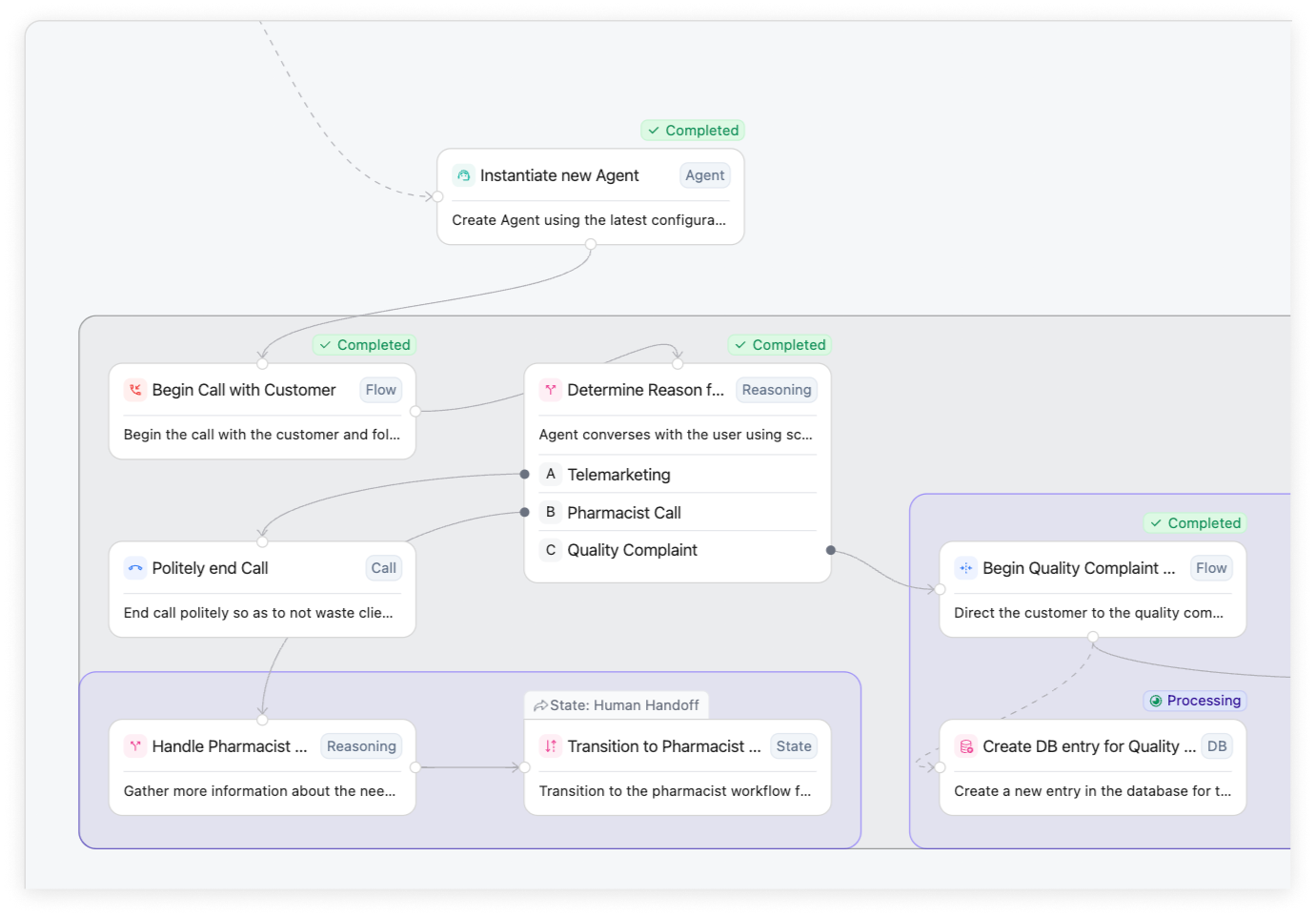
Configure Tensor to match your unique processes
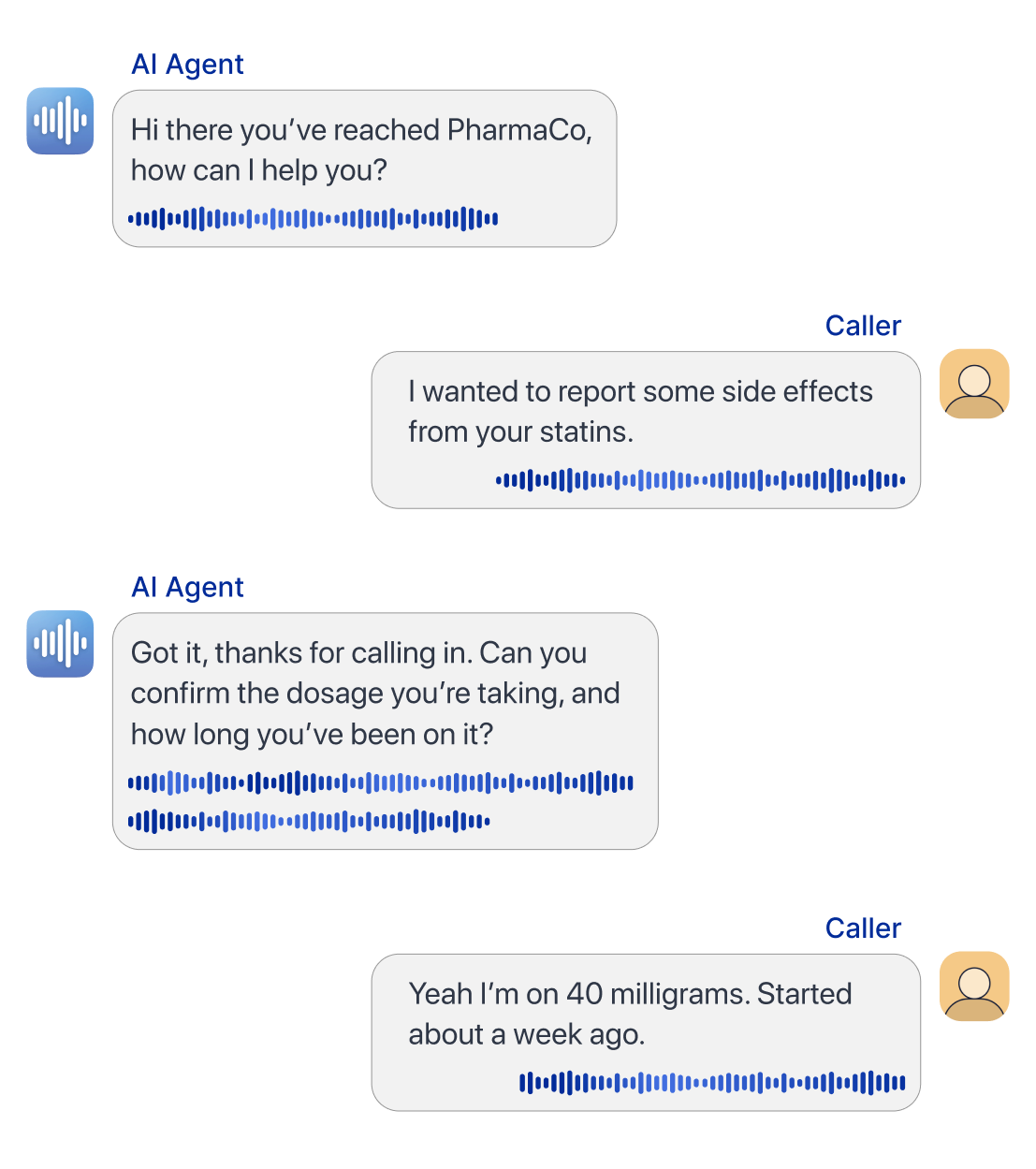
Tensor AI Agents handle up to 99% of phone calls with no human intervention
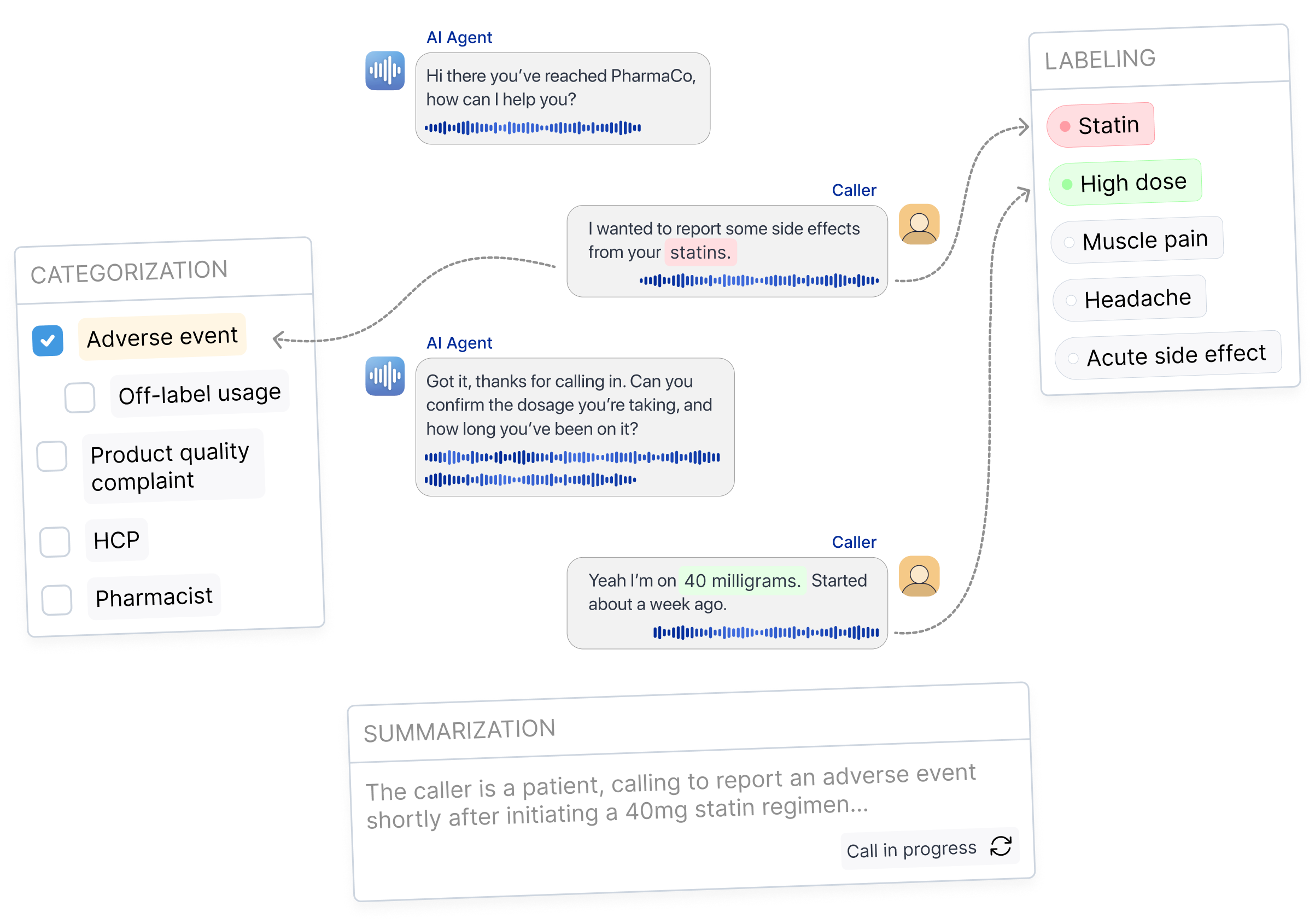
For every call, Tensor can:
These annotations add structure and clarity to an ocean of data to help you uncover new insights to improve your business
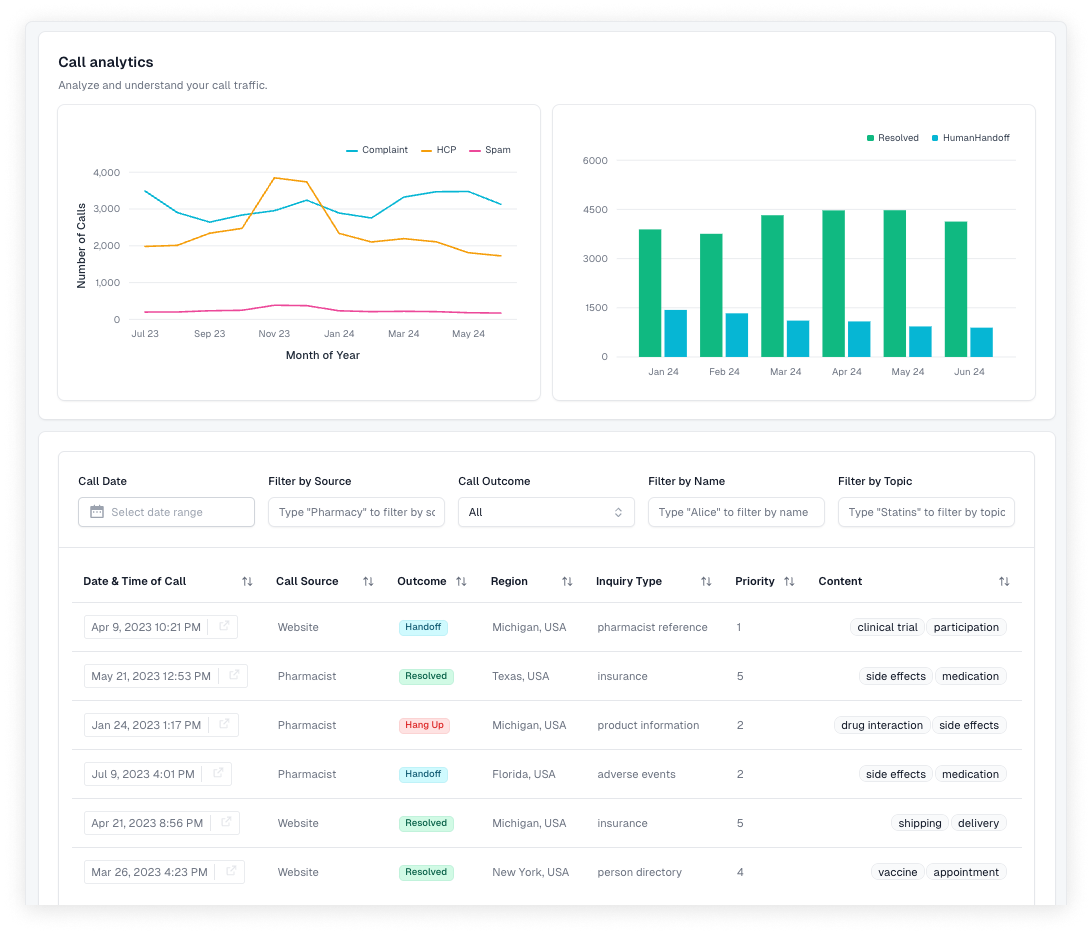
Tensor’s reporting and analytics serve two goals:
AI phone call automation provides a rare opportunity to slash costs while simultaneously boosting HEDIS and uncovering new insights to improve your practice

Tensor’s AI communicates with your EHR, CCaaS, ERP, and CRM systems as needed to successfully resolve any call
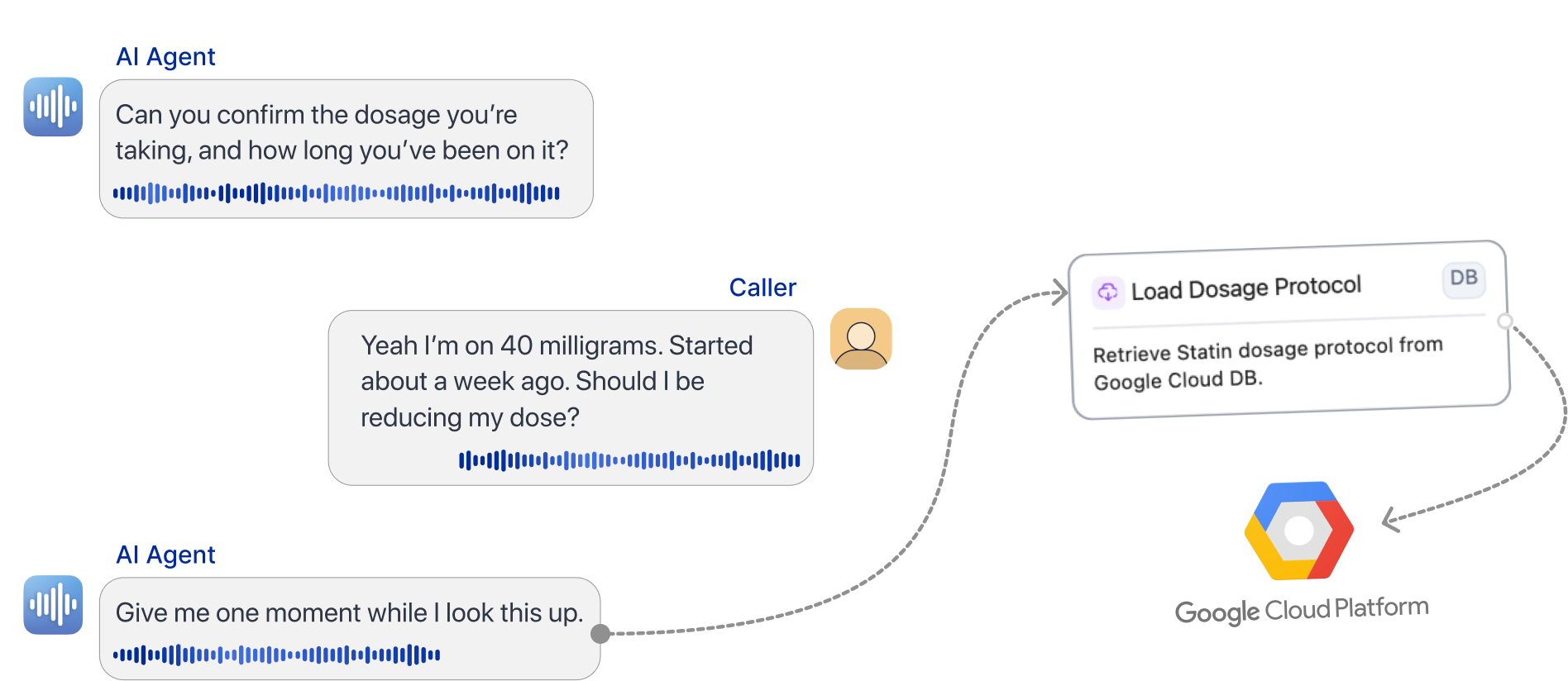
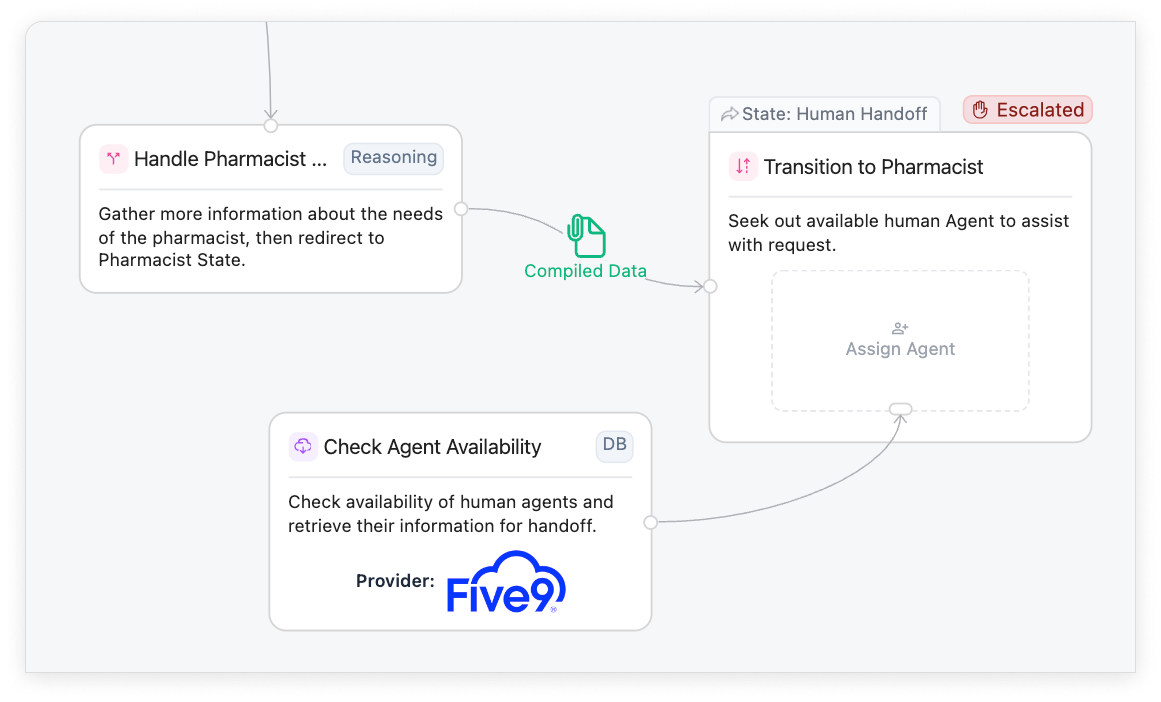
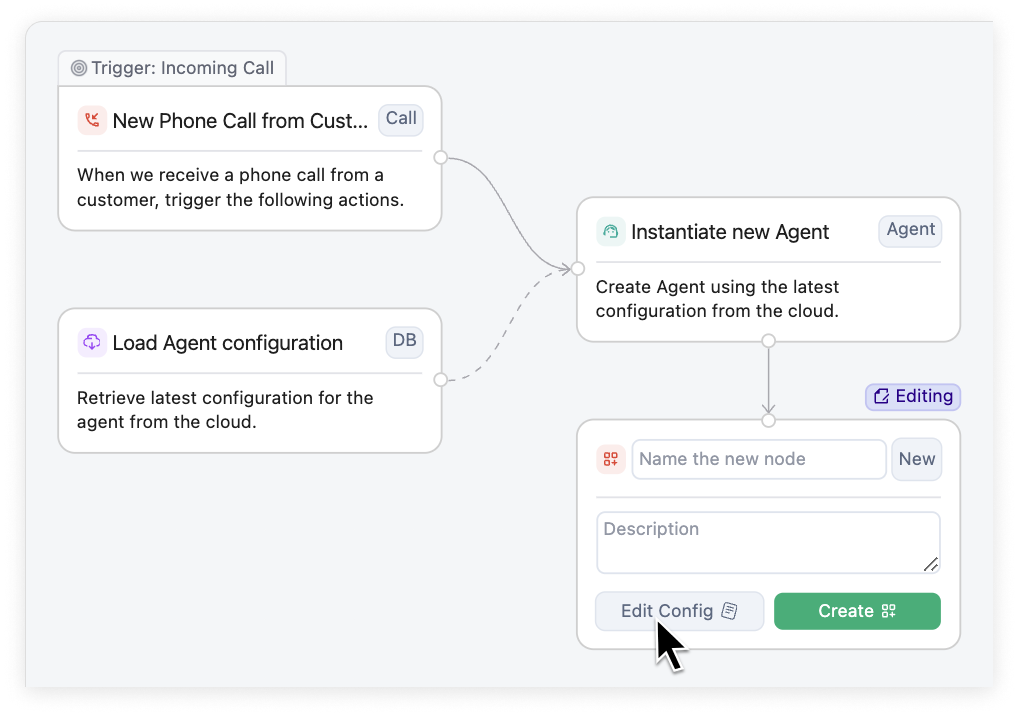
As your business changes, so must your call center workflows
Tensor is built for rapid deployment & iteration, and gives you the ability to:
Sensitive data requires a careful approach and robust processes. We take security and process integrity seriously – and it shows. As part of our goal to be the most secure and reliable tool in our customers’ arsenal, we offer HIPAA compliance, HITRUST and SOC 2 certification.

AI phone call automation provides a rare opportunity to slash costs while simultaneously boosting HEDIS and uncovering new insights to improve your practice
Tensor is trusted by visionary healthcare leaders
Tensor has transformed the way our team manages prior authorization. Its gone from Excel sheet chaos to streamlined and automated. Saves my team hours a day.

COO, trüHealthNow
Love the product and the team. They flew out to our offices, sat with our medical billers to deeply understand our workflows. Then they tailored the product to our needs. It's been a game changer.

CEO, Physicians Choice Medical Billing
Exploring the innovations that help healthcare organizations thrive